There are a number of different job opportunities available in the healthcare market, thanks to lightning speed advancements in the medical technology field. Many healthcare career opportunities did not exist twenty to thirty years ago. However, with more people requiring medical attention, and new insurance regulations, there is a demand for qualified and trained medical billing and coding professionals. Did you know medical billing is one of the fastest-growing health care professions today?
If you’re interested in training for a new career in the healthcare field, explore the healthcare training programs offered by U.S Colleges. Our programs are short-term, allowing you to earn a diploma in less than 16 weeks!
WHAT IS MEDICAL BILLING AND CODING?
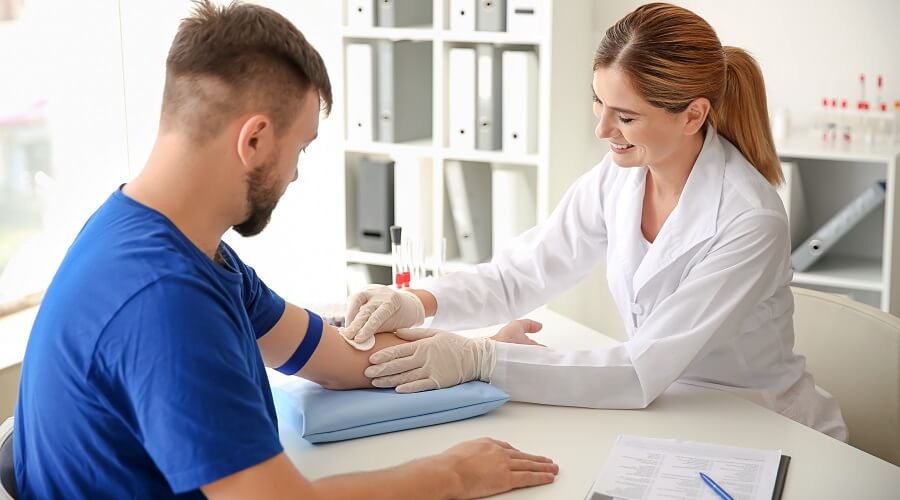
When we go to the doctor’s we mostly pay attention to the medical assistant and the doctor, after all they are the ones we interact with, but they are not the only ones making sure we have the best possible treatment. We are probably too busy worrying about our health ailments to notice the men and women working in the background making sure our medical claim are being processed and billed correctly.
Medical coding and billing are two separate tasks, handled by different individuals. However, in some small doctor’s office, a single individual can handle both duties, as well. For this reason, the more training and preparation a medical billing and coding professional receives the more successful they will be on the job. So what is the difference between a medical biller and a medical coder?
Medical coder’s main role is to decode the service or procedure written on the patient’s documentation provided by the healthcare provider, and then determines the appropriate procedure (CPT) and diagnosis code to submit. Medical coding workers spend time in assessing and properly coding the data, in order to ensure an accurate billing procedure is free of any errors.
Then, the Medical Biller inputs the claims with the appropriate codes and submits the claim to the insurance company for billing. The medical biller then follows-up with the insurance company to make sure the claim has been approved, if there are any discrepancies or missing information, they reach out to the patient and let them know what is happening with their claim.
CAREER GROWTH OPPORTUNITIES
Medical coding and billing professionals are essential in order for hospitals and other medical institutions to run effectively and efficiently. It is imperative that patient records and billing matters are handled proficiently and with the up-most integrity.
According to the Bureau of Labor Statistics, new job opportunities for recently trained medical billing or medical coding professionals is growing much faster than the average for all other professions. The demand for health services and trained healthcare professionals is expected to increase as the population ages and life expectancy keeps extending.
Medical billing and coding qualified and trained professionals have the opportunity to seek employment at hospitals, private clinics, health insurance companies, nursing care and rehabilitation facilities, or medical billing companies.
MEDICAL BILLING AND CODING TRAINING
If you are serious about entering the medical billing and coding field, then you must undergo proper training and certification. Medical billing and coders typically need post-secondary training.
Achieving this feat is rather easy; all you have to do is register into a medical billing & coding program at the college of your choice. Once you complete your short training, you can start applying for jobs at any medical facility. Easy right, so what are you waiting for?
PS. For a full list of our high in-demand healthcare training programs check out our healthcare training programs page. And if you can’t wait another minute to get started on your future call the number in the upper right-hand corner of the website to speak with an admissions specialist today.